Inside access: Future horizons in interventional radiology
Room considerations for a telerobotic angiosuite
Future Horizons in Interventional Radiology. Gaba, Ron C. et al. Journal of Vascular and Interventional Radiology, Volume 36, Issue 12, 1825.
The December issue of Journal of Vascular and Interventional Radiology explored the question of which unique and pioneering ideas of today will become the routine IR procedures 1–2 decades from now? This special section, guest edited by the 2024–2025 JVIR Resident Editorial Fellows—Vishnu Chandra, MD, Rebecca Le, MD, Mohammad Mirza-Agazadeh-Attari, MD, Anne Sailer, MD, and Avik Som, MD, PhD—included 19 mini-review articles (Research-in-Translation format) explore the most promising IR science that may translate to the next clinical breakthroughs.
IRQ spoke with one of the guest editors, Dr. Rebecca Le, on her experience with the special issue.
Tell us about you, your team, and your institution.
Rebecca Le, MD: I graduated from Emory University IR/DR residency in 2025 and am in private practice as an attending in northern California. When the JVIR editorial fellows were organizing this special issue on translational medicine in interventional radiology, I recruited founders from the Biodesign & Innovation of Minimally Invasive Technologies (BIMIT) Lab (Drs. Hanssen Li & John Moon) specifically to discuss the role of telerobotics in interventional radiology.
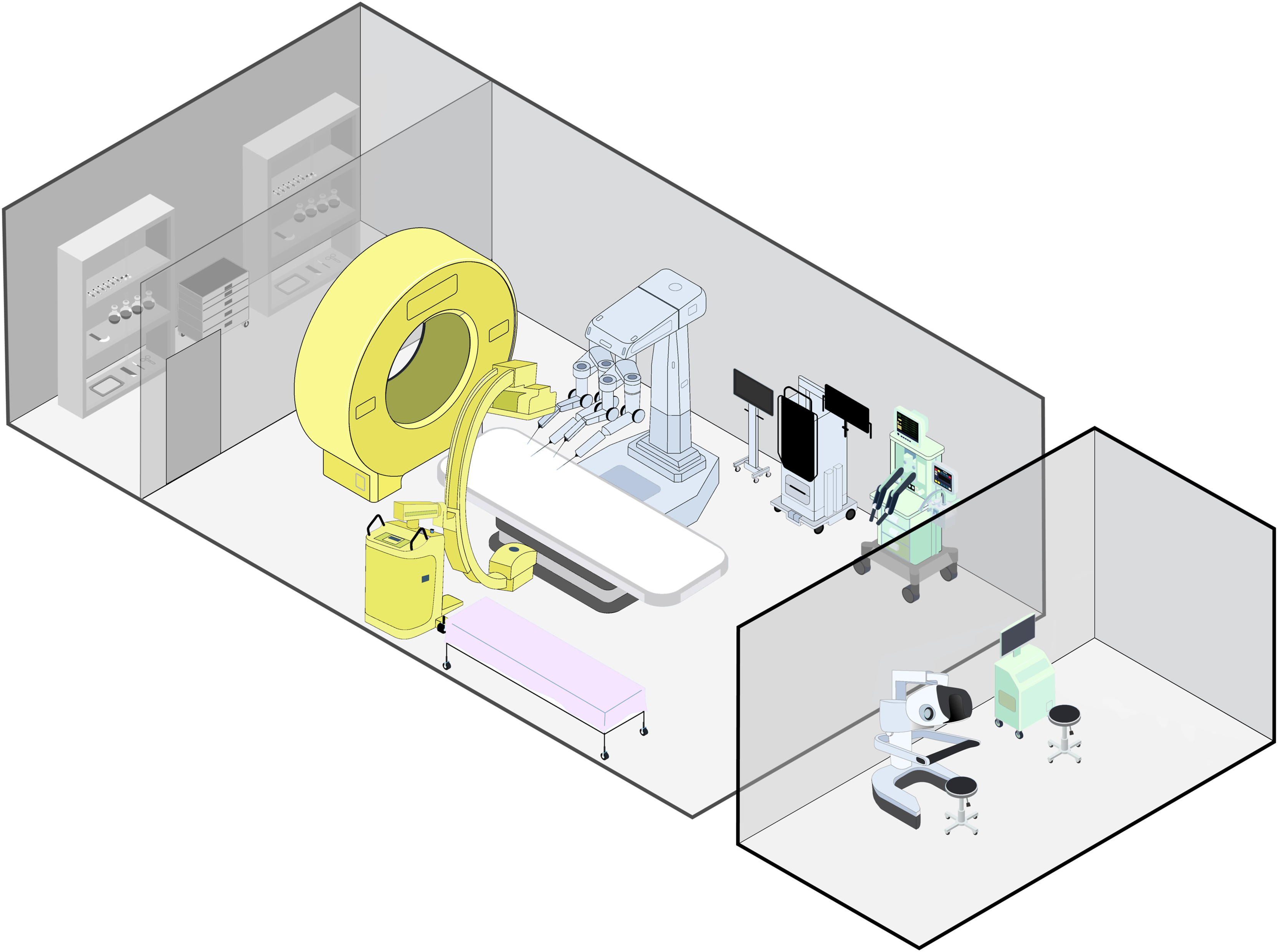
Why did you pursue this topic?
Dr. Le: There are not enough interventional radiologists in the world to take care of patients, and there should be discussion and strategic development for ways to lessen this burden.
What are the key takeaways from this research?
Dr. Le: Telerobotics is a feasible option that could be pursued to provide interventional radiology services in areas of critical need.
How might this research influence treatment, practice, or clinical processes in interventional radiology?
Dr. Le: This research would help lessen health disparities by improving access to care.
What challenges were faced while translating this research into practical applications, and how did you overcome them?
Dr. Le: Cost and reliability of networks to promote robotics remain key barriers in full-scale adoption. Networks for optimized remote and secure connections are essential from a patient safety perspective. These are high priority areas of research that are currently being studied in order to facilitate positive moments of telerobotics into the community, outside of ongoing research to improve telerobotic procedures.
Which emerging technologies or methods do you believe hold the greatest potential to shape the future of IR?
Dr. Le: A tele-angiosuite has the potential to bring access to patients where there is a critical shortage or absence of providers. From an IR standpoint, this would require IRs to learn new additional skillsets to operate in a tele-angiosuite, adding more tools in our ever-evolving toolbox.
How do you envision the adoption of your findings impacting patient care or outcomes in the next 5–10 years?
Dr. Le: What might be possible for telerobotics is contingent on cost. Technology is improving daily—the next step involves research to ensure that telerobotics can be performed reliably and safely. In advance of research to advance procedures in telerobotics, such as arterial access, arterial selection, etc., research in optimizing the infrastructure must be performed in tandem.
