SIR Today
A novel approach for improving hyperglycemia in type 2 diabetics
An SIR 2026 Abstract of the Year
T. Pan, Q. Zhang
Patients with type 2 diabetes mellitus may experience significant improvement in hyperglycemia following endovascular denervation (EDN) with a novel six-electrode catheter system, a new study shows.
“Study of MultI-eLectrode EndovaScular DenervaTiOn in PatieNts with Type 2 Diabetes MEllitus (MILESTONE): 6-month Analysis from the First-in-human Proof-of-concept Study,” one of the SIR 2026 Abstracts of the Year, assessed the safety and glycemic indices following EDN for 11 patients with Type 2 Diabetes Mellitus (T2DM).
“T2DM imposes a substantial global health burden, with the worldwide prevalence of chronic hyperglycemia or diabetes affecting approximately 1 in 11 adults,” said Tao Pan, MD, PhD, lead author of the abstract. “Standard management strategies for T2DM include dietary control, physical activity, weight management and pharmacological interventions. Unfortunately, despite the availability of a wide range of pharmacological options, achieving adequate glycemic control remains a major challenge.”
According to Dr. Pan, this is primarily due to poor patient compliance with complex medication regimens and the intricate pathophysiological mechanisms underlying T2DM. Therefore, he believes that investigating whether EDN can provide a direct and effective approach to improving glucose metabolism—and thus offer a novel therapeutic modality for T2DM—holds significant clinical value.
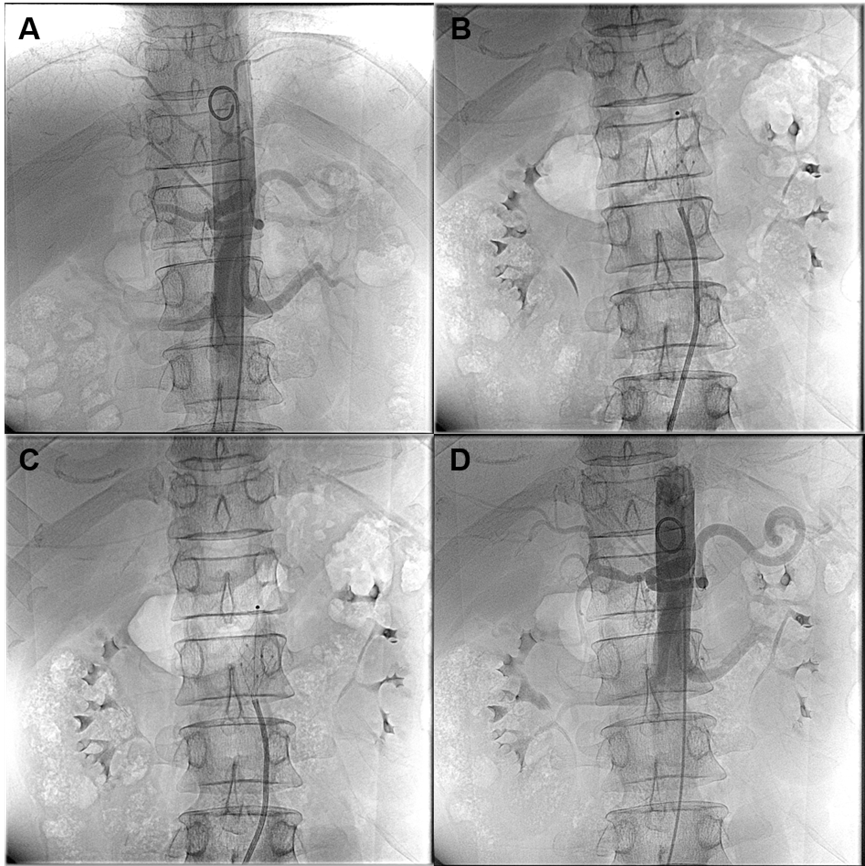
Exploring a novel therapy
“Chronic overactivation of the sympathetic nervous system (SNS) has been identified as a key factor inducing insulin resistance, which in turn contributes to the development of T2DM and metabolic syndrome. Consequently, catheter-based renal denervation (RDN) has been tentatively explored, as it has been proposed as a potentially effective intervention for treating resistant hypertension and associated metabolic disorders,” Dr. Pan said.
However, previous investigations into the effects of RDN on blood pressure and insulin sensitivity in patients with metabolic syndrome have failed to demonstrate improvements in fasting glucose, insulin sensitivity or sympathetic activity.
“This lack of efficacy is presumably attributed to insufficient denervation, leaving the role of RDN in T2DM treatment controversial,” Dr. Pan said.
The impact of a multi-electrode catheter system
Dr. Pan and his co-author, Qi Zhang, MD, PhD, both of Zhongda Hospital, Southeast University, sought to build on their prior research evaluating the effects of multi-electrode catheter-based RDN on insulin sensitivity and glucose metabolism in a canine model. Using a novel six-electrode catheter system, EDN was conducted on the celiac artery (CA), and aorta between CA and the superior mesenteric artery (SMA) on 11 patients. Special consideration was given to patients with comorbid metabolic syndrome or metabolic-associated fatty liver disease (MAFLD).
The novel catheter system is a multi-electrode artery radio-frequency ablation system comprised of the multi-electrode artery radio-frequency ablation catheter and the multi-electrode artery radio-frequency generator, Dr. Pan said. During the EDN procedure, the six-electrode catheter was inserted to CA and aorta between CA and SMA through the sheath.
“Each ablation catheter electrode forms a closed loop between the inner wall of the blood vessel and the circuit electrode, which releases radio-frequency energy and increases tissue temperature to the sympathetic nerve fibers in the artery wall, to achieve the purpose of ablation and damage of sympathetic nerves,” Dr. Pan said. “This ablation would result in the blocking or partially blocking of sympathetic nerve signal transmission and reducing the excitability of the sympathetic nerve.”
A technical success
Researchers evaluated safety, HbA1c levels, homeostasis-model assessment of insulin resistance and fasting plasma glucose. Antidiabetic medication, lifestyle, physical condition, blood pressure and plasma biochemistry were also recorded.
Data indicated a 100% technical success rate, with no severe treatment-related adverse events or major complications were observed. Researchers identified that both HbA1c and HOMA-IR significantly reduced at 6 months and also observed a reduction of daily insulin rejection without changes in lifestyle.
“This study suggested that EDN using the novel six-electrode catheter system at the new sites of CA and aorta between CA and SMA elicits a clinically significant improvement in hyperglycemia in patients with T2DM, with good tolerability,” Dr. Pan said. “Achievement of such metabolic benefit through a minimally interventional treatment offers a potentially new therapeutic solution for patients with T2DM.”
The EDN approach may overcome treatment adherence and compliance issues, a major shortcoming of all pharmacological approaches, he said.
“Beyond hypertension and diabetes, all diseases associated with sympathetic nervous system overactivation represent potential targets for EDN intervention,” Dr. Pan said. “We anticipate that additional clinical research will be undertaken to explore these avenues, ultimately providing novel insights and innovative approaches for the treatment of such conditions.”
